Dr. Marleen Groenier1, Dr. Ir. Jasper Homminga1, Dr. Frank Halfwerk1,2
- Technical Medicine, University of Twente
- Department of Cardio-Thoracic Surgery, Thoraxcentrum Twente, Medisch Spectrum Twente
Becoming a technical physician: Scientific foundations and educational principles
Preface
Healthcare is transforming rapidly because of medical technology. The rising gap between more complex healthcare and technology cannot be filled by traditional medical doctors and engineers. Healthcare professionals with specific technical-medical expertise are needed, i.e., technical physicians, for safe, efficient and effective use and optimization of medical technology in direct patient care. In this chapter, we explain why healthcare professionals who work with medical technology need specific technical-medical expertise, what technical-medical expertise is (and is not) and describe the underlying evidence-based educational principles for a technical medicine curriculum. Because technical physician, or technical-medical doctor, is an emerging profession in healthcare, technical physicians need to be able to position themselves as healthcare professionals with complementary competencies and an independent authority in patient care. Technical physicians need to establish personal relationships and trust in competencies to be able to practice technical medicine in clinical practice.
Background
Medical technology is rapidly being introduced in healthcare and most of the important innovations in medicine are technological in nature.[1] A further increase in technology use in healthcare is anticipated,[2] thus creating opportunities for tailoring such technologies to patient-specific needs. However, traditional medical school curricula primarily train physicians to diagnose illness and manage treatment pathways.[3] So far, existing medical curricula inadequately equip physicians to evaluate the clinical significance of medical devices, modifications in the use of medical devices, or innovative approaches in medical technology use for treating patients.[3][4][5] Indeed, conventional medical curricula insufficiently provide students with the knowledge, skills and tools to utilize and adapt technology safely in clinical practice and improve the efficiency of healthcare delivery.[6] These rapid technological and societal changes combined with a lack of physicians’ technological knowledge and skills result in suboptimal and misuse of medical technology, sometimes even resulting in adverse events.[7] To prevent the suboptimal use and certainly misuse of technology in healthcare, we need to educate healthcare professionals with specific technical-medical expertise.[8][9]
In this chapter, we discuss the similarities and differences of expertise development in the engineering and in the medical domain as well as the implications this has for defining expertise in the technical-medical domain. Furthermore, the difference between routine, adaptive and interdisciplinary expertise is explained. Next, evidence-based educational principles are presented that support technical-medical expertise development. Lastly, future directions are presented.
How do you become an expert?
Expertise, or expert performance, is defined by Ericsson and Lehmann[10] as “consistently superior performance on a specified set of representative tasks for a domain” (p. 277). It usually takes years of extensive experience in a particular domain to reach such an expert level of performance.[10][11] In general, expertise comes with great advantages.[12] Experts can rapidly detect relevant information, have successful self-monitoring skills, are effective problem-solvers and can generate the most satisfactory solutions.[12] Although novices and experts often use the same problem-solving or reasoning processes, experts are quicker and more effective at solving routine problems in their own domain.[13] Through experience, they have gathered a large body of knowledge over time which results in a change in knowledge organization and use.[10][14] Experts’ particular knowledge organizations allow them to perceive large meaningful patterns, represent professional situations at a deep, more abstract level[13] and show, among others, superior performance in short-term and long-term memory, and self-monitoring skills.[13]
According to Ericsson[11] and Ericsson and Lehmann[10], the key to reaching expert performance lies in deliberate practice, which is the deliberate attempt of an individual to increase performance by avoiding “arrested development associated with automaticity” (Ericsson[11], p. 991). Deliberate practice consists of repeatedly performing activities that are specifically designed to successively improve and refine domain-specific skills. A typical example is a high-performing athlete who is guided by a coach and whose training is specifically targeted at deficiencies in performance.[15] Fadde and Klein[16] state that although deliberate practice by professionals works out in some fields, such as music and sports, it seems impractical to expect professionals to practice in addition to doing their jobs. Also, deliberate practice might be useful for routine practical (clinical) activities, e.g., becoming better at suturing and improving the interpretation of scans, but might be less applicable to cognitive and mental tasks, e.g., coming up with alternative ideas or solutions to a problem. Fadde and Klein[16] further explain that professionals can perform small mental exercises while on the job, such as predicting the outcome of a lab test, which is called deliberate performance. Deliberate performance is believed to enhance reflective practice, which supports career advancement and improves the success of an organization or team.[16]
Although expertise in general comes with many advantages, there are also drawbacks to being an expert. Research has shown that expertise is domain-specific.[12] This can guide experts to apply solutions or routines that worked in previous situations to situations that are non-routine while overlooking the greater complexity of these non-routine situations. An expert can develop a narrow perspective and might miss out on insights and new ideas from other fields. Having an elaborate and well-organized knowledge base in combination with rapid pattern recognition can also lead to ‘filling in the blanks’ when working on a problem and thus jumping to conclusions too soon.[17] Also, experts may be resistant to new ideas or changes in their field. The routines that experts develop might become outdated when tasks and professional practice change. Because they invested a large amount of time and effort in becoming proficient in their field, experts might resist innovation and adaptation of their professional practice.[18][19]
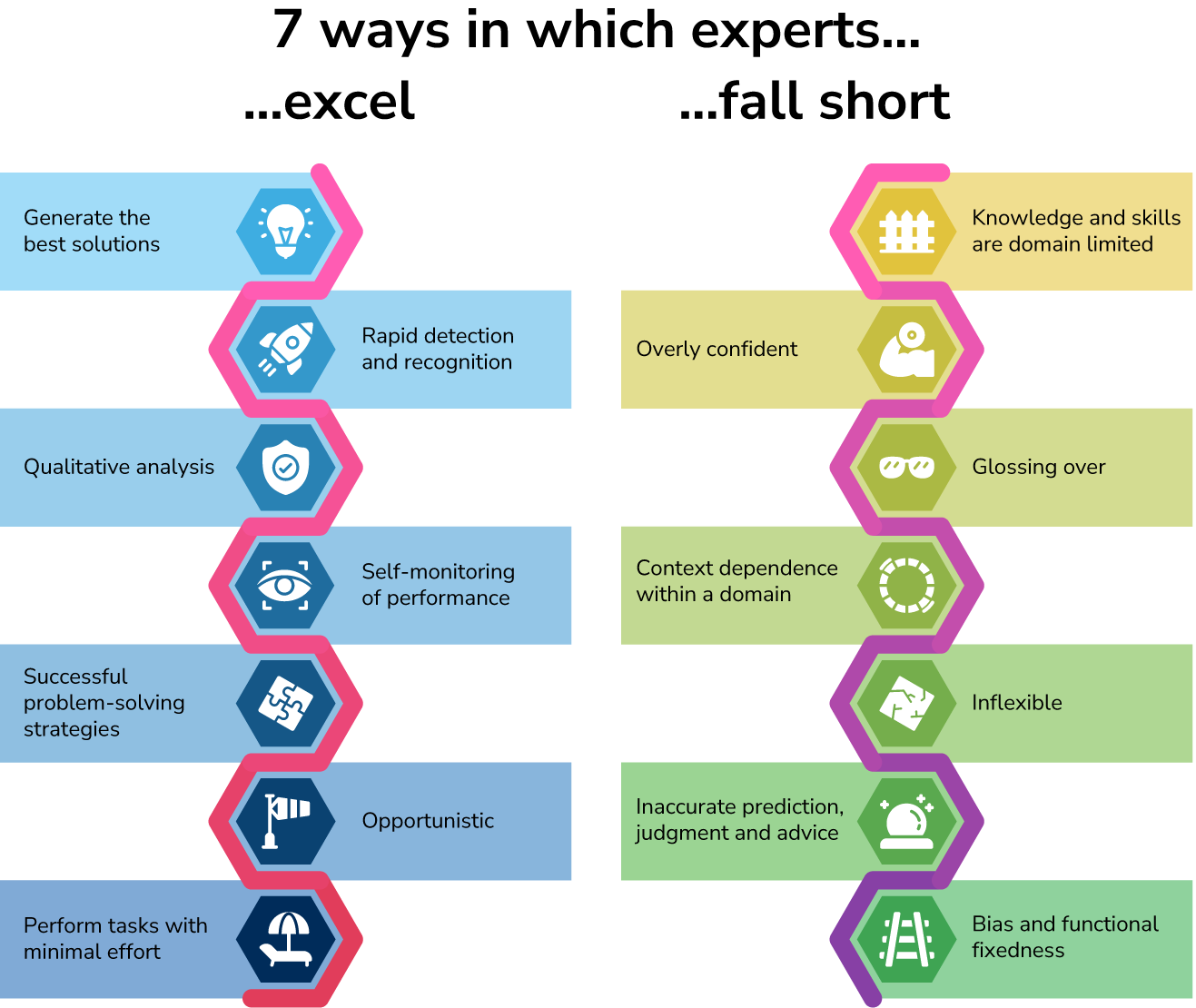
To summarize, experts show excellent, consistent performance in their field using their experience, large body of knowledge and automated routines. Experts use deliberate practice with a coach during training or perform small mental activities on the job (deliberate performance) to further refine their skills. A pitfall of expertise is that experts might miss out on important, different perspectives and become resistant to change. The ways in which experts excel and fall short are summarized in Figure 1.
Clinical reasoning and medical expertise
In clinical practice, physicians are frequently faced with questions such as: what is the diagnosis for this patient? Which treatment is most effective given this patient’s condition? They are confronted with diagnostic or treatment selection problems (also called categorization problems[20]). Knowledge about concepts, such as blood pressure, fever and tachycardia, and their interrelations are required to solve these problems adequately.[21] Clinicians learn to find regularities in patterns of features, such as complaints and symptoms, and interpret them. By solving categorization problems over and over again on the job, clinicians develop illness scripts: structured ways of organizing and storing knowledge.[22]. Illness scripts are mental representations of knowledge and allow clinicians to quickly process information and, most of the time, help to make accurate decisions.[23]
Mylopoulos et al.[24] argue that research has focused too much on how clinicians diagnose patients in the investigation of expertise and expertise development. This has led to the perception of an expert clinician as a highly skilled diagnostician who can apply a set of routines effectively and efficiently in practice. The result of this emphasis on diagnostic excellence on routine problems is that this has led to “educational models for equipping our novices with more intellectual resources faster.” (Mylopoulos et al.[24], p. 1162). In medical education, the focus is still mostly on acquiring automated routines as quickly as possible through repeated exposure to clinical cases, and sometimes on basic communication or technical skills. There is a strong focus on mastering existing knowledge and techniques.[25]. According to Mylopoulos et al.,[24] this narrow focus has also influenced how training and practice are organized until now and our ideas of who can be considered an expert.
Engineering expertise
Engineering expertise involves the ability to identify and solve complex problems through a systematic and analytical approach. A broadly educated engineer is a creative thinker, engaged with complex societal problems and has the technical and social competencies necessary to work on solving these problems.[26] Engineers are problem solvers with a problem analysis approach, more specifically they solve design problems, e.g., how can we waste less water in the shower? Solutions to these design problems take the form of new plans, protocols, or artifacts, for example, a water-saving showerhead.[21] The design process is characterized as a set of activities to create a working solution(s) for diverse societal-technological challenges and opportunities.[26] These activities are methodically planned, transparent, and either iterative or sequential.[26] Koen[27] defines the engineering design method as follows: “The strategy for causing the best change in a poorly understood or uncertain situation within the available resources” (p. 10).
Traditional medical problem-solving is essentially different from solving design problems, according to Goel and Pirolli.[28] The steps are different as well as the underlying knowledge representation needed to solve the problem. Engineers design and analyze systems, structures, devices, and processes to meet specific goals and requirements. They need conceptual knowledge to solve these design problems, i.e., knowledge about concepts and interpretations of these concepts.[21] An engineer needs to understand the underlying principles used but also the functional requirements: what is the designed solution supposed to do? These solutions are usually innovative and the design process often means taking risks, experimenting and failing; something might not work as expected. A key characteristic of designing in engineering is the use of failures and unforeseen situations to adapt.[3] This contrasts with the working habits of clinicians, who avoid risks (as they might harm a patient) and experimentation is strictly regulated.[29][30]
Technical-medical expertise
Medical technology offers new solutions for clinical problems: new ways to diagnose, treat or rehabilitate patients. However, these clinical problems involving the use of technology can be considered complex and non-traditional; they can be described as design problems.[9] An example of a technical-medical design problem is: how can we monitor the harmful mechanisms of mechanical ventilation and adjust the ventilation to what this specific patient needs, while minimizing the harmful side effects? To solve these technical-medical design problems experts need to be able to recognize when a clinical problem is non-routine, i.e., outside the scope of the physicians’ expertise, think like engineers and be able to innovate clinical routines in direct and indirect patient care.
Technical-medical experts’ problem-solving therefore begins from the patient’s perspective, like a physician, while at the same time assessing possible uses and consequences of medical technology, like an engineer.[9] Underlying technical-medical expertise is “an understanding of medical technology use as the complex interaction between the human body and the technologies’ underlying principles” (Groenier et al.[9], p. 623). It means translating and integrating knowledge and skills between the technical and medical domains.[9] Specific technical-medical expertise is needed for innovative and safe uses of technology in healthcare to optimize diagnosis, treatment and rehabilitation.
Adaptive expertise
Technical medicine is an emerging field with currently only a few role models. It is an interdisciplinary, hybrid field at the intersection of the technical and medical domains, transforming traditional medical practice. According to Palonen et al.[31], adaptive expertise is most important in emerging or hybrid fields because experts in these fields need to be able to move flexibly from one area to the next and be able to integrate these. Also, professionals in emerging domains develop new problem-solving strategies on the go and without available role models they need to define their own professional identity. In technical medicine, effective transfer of knowledge and skills between these domains should take place to bridge the gap between engineering and medicine.

Adaptive expertise is characterized by balancing innovation and efficiency, see Figure 2.[32][33] Even in non-routine, unfamiliar situations, adaptive experts maintain a high level of performance based on understanding why certain actions are useful in certain situations.[34] Similar to engineers, adaptive experts have deeper conceptual knowledge. To perform adaptively, i.e., knowing when your knowledge and skills are insufficient and new ways of thinking and working are needed, requires resilience, adequate self-regulation skills and self-insight.[34] Critical thinking and reflection support this adaptive performance and awareness of the limitations and strengths of one’s knowledge and skills.[35] Taken together, adaptive expertise is more than extended knowledge and skills, it is a mindset that reflects cognitive flexibility, creativity and an openness to new and different perspectives. The rise of disruptive technology use in medicine urges professionals to change from knowledge-based expertise to adaptive and interdisciplinary expertise.
Interdisciplinary expertise
A notion similar to adaptive expertise is interdisciplinary expertise. Boon et al.[36] define interdisciplinary expertise as “the cognitive ability to integrate or combine knowledge from different sources and to transfer knowledge from one domain to another such as to generate new knowledge for novel problems.” (Boon et al.[36], p. 670). Interdisciplinary expertise seems to overlap with adaptive expertise. However, it is a broadening of the concept of adaptive expertise and the consequences of this distinction are relevant for technical medical education.
Interdisciplinary collaboration requires a specific type of expertise, in line with adaptive expertise.[36] Underlying interdisciplinary expertise is the ability to understand cognitive and epistemological issues of different domains. Interdisciplinary experts can make connections between or integrate knowledge and methods from other disciplines to come up with new, innovative solutions. According to Boon et al.[36], this is different from adaptive expertise because experts in interdisciplinary fields not only need to acknowledge that knowledge from domains needs to be integrated, but they also need to recognize the workings of disciplinary perspectives. These disciplinary perspectives or paradigms determine how experts in a particular domain define knowledge and how knowledge is constructed, see Figure 3. Disciplines such as medicine and engineering have very different hidden or implicit disciplinary perspectives that cannot easily be communicated which makes effective collaboration between these disciplines inherently difficult.[36]

To conclude, engineers, physicians and even technical physicians ‘see’ different aspects of a clinical problem, based on their own disciplinary perspectives. Making technical medicine students aware of these different disciplinary perspectives and how they influence the generation of knowledge in clinical practice is a first step towards the development of interdisciplinary expertise.
Teaching for technical-medical expertise development
Medical schools struggle to incorporate technical competencies into their curricula (Green). Some more recent medical education programs introduce the engineering or design thinking approach in their curriculum to teach students how to develop new devices or technical innovations, e.g., prototypes or e-health applications (see e.g., Overton et al.[6]). MD/MEng programs are developed for medical students to “acquire technical interdisciplinary skills that bridge the gap between clinical medicine and the increasingly demanding technological dimensions of the healthcare environment.” (Rambukwella et al.[3], p. 897). Another approach is the ‘layered-on’ method which means that medical and engineering degrees are stacked or joint degrees are created. These medical curricula add a biomedical or clinical engineering focus, often combined with entrepreneur, business or healthcare management skills. The question remains if these students with double or joint degrees are able to connect these domains because courses and programs are offered without integration, and therefore possibly also limiting the interdisciplinary growth potential of students.
Teaching medical students or other healthcare professionals design thinking, the engineering problem-solving approach or a positive attitude to innovating in clinical practice will lead to more technology successfully introduced into healthcare because the end users are now really part of the design process. However, these initiatives do not resolve the problem of the misuse or suboptimal use of technology in healthcare because they focus on the design of technology instead of its application in direct patient care. In clinical practice, healthcare professionals actually often experience a lack of knowledge and skills to use technology safely, efficiently and effectively, even those who work in technology-intensive disciplines, such as radiology.[2] Evaluation of technical innovations in medicine is also still frequently lacking. To counter the suboptimal and misuse of technology, healthcare professionals need a thorough understanding of the core technical principles underlying medical technologies, i.e., how magnetism, light, sound or radiation work and interact with the human body.
In contrast, a technical medicine curriculum is fundamentally different than the ‘layered-on’ method, i.e., stacking degrees or joint degrees, or a biomedical engineering curriculum. The technical medicine curriculum developed at the University of Twente aims at innovating diagnosis, treatment and rehabilitation of individual patients in direct patient care using technology, often developed by biomedical engineers. Indeed, the program does not result in an engineer with some medical background or a physician with some technical background, but in a technical-medical doctor.
Being a technical physician means translating technological principles and approaches from the engineering domain and being able to apply them in direct patient care with individual patients. This requires the ability to flexibly adapt acquired knowledge and skills and learn from applying knowledge and skills to novel, non-routine clinical problems. This ability is also called adaptive expertise. For adaptive expertise development in the technical-medical domain, in-depth conceptual domain knowledge, the ability to think like an engineer, and a reflective attitude and willingness to learn are essential.
Educational principles
Cognitive integration
Cognitive integration is a learning strategy that supports the acquisition of conceptual knowledge.[37] Cognitive integration is most effective by building associations between concepts and linking concepts in causal relationships.[38] For example, at the program level, learning facts and theory is intertwined with the (clinical) application of that knowledge, e.g., in authentic, representative technical-medical projects resulting in high levels of understanding of technology and medical concepts. Contextualizing the theoretical knowledge in such projects helps students link different concepts with each other. This should, however, be done in various contexts to ensure that students learn the underlying principles and abstractions instead of just the concrete examples.[38]
Cognitive integration is most strongly reflected in the TM heuristic, meaning a method of learning or solving problems that allows people to discover things themselves and learn from their own experiences.[39] The TM problem-solving process starts with an analysis of anatomy, physiology, pathophysiology and technology. Cognitive integration, resulting in having a deep understanding of a subject and the ability to apply this knowledge successfully to new problems, is supported by teaching each subsystem of the human body using the TM heuristic.
Project-based learning
Engineering problem-solving is quite similar to design problem-solving. Rambukwella et al.[3] note that “one approach to understanding technology and innovation is through design thinking and project-based learning” (p. 899) Project-based learning supports the research-based design or engineering process. This research-based design process involves bringing research and practice closer together by engaging practitioners in the co-creation of new knowledge.[40] The starting point of research-based design is a thorough analysis to define the problem for which a solution needs to be designed. This systematic and analytic engineering approach to analyzing and defining the problem aligns well with the deliberate use of medical technology.[9] The design process that students can experiment with in project-based learning also requires creativity and courage.[9][41] Project-based learning, when implemented well, helps students perform as well as or better than traditional learners in high-stakes tests, improves problem-solving and collaboration skills, and improves students’ attitudes toward learning.
Reflective practice
Critical reflection on (professional) experiences is one of the most important learning processes to support professional and personal growth as well as expertise development.[16][42] According to Schön,[42] experimentation is essential to developing reflection-in-action, i.e., the consistent and constant reflection on the intervention or action while it is happening. Technical-medical students and experts learn from trying new ways of doing something, reflecting on the outcomes, and adopting, rejecting or adapting this new way of working during their multiple clinical rotations in various hospitals. This approach is similar to that of scientist-practitioners, who use their own practices as experimental situations and put the scientific method into clinical practice.[43] There is the risk of over-automating practices by repeated exposure to similar clinical situations. To counter this unreflective automaticity in performance, technical-medical students and experts should be encouraged to create learning moments in their day-to-day practice by deliberately experimenting with new ways of working and have more opportunities for reflection-in-action.[16]
Simulation-based learning
Simulation offers dedicated learning opportunities to complement the traditional work-based learning environment. In a simulated environment, there are ample possibilities to implement learning strategies, such as deliberate practice,[44] that contribute to adaptive expertise development. Exercises can be easily be repeated and allow for a variety of clinical situations and approaches guided by expert-, peer- and self-observation. Also, timely feedback on the process can be easily implemented (rather than feedback on the result) by the use of nonexpert, unambiguous measures such as time to complete a task, self-generated judgment or technology-supported performance metrics. In addition, task difficulty can be varied and progressively more difficult tasks or challenging situations can be introduced according to the learner’s needs (see Fadde and Klein[16] and Ward et al.[45] for an overview of learning strategies for adaptive expertise development).
The major advantage of simulation-based learning in technical-medicine is that students can experiment with various ways to perform technical-medical procedures without risking harm to the patient; they can demonstrate proficiency before practicing on patients.[46] In a safe learning environment, there is room for making mistakes and learning from them, thus increasing confidence, a positive attitude towards learning, and developing new ways of thinking and working (adaptive expertise).
Many training programs in simulation centers adopt the traditional ‘see one, do one, teach one’ teaching approach. Trainees are instructed by experts and have to follow these instructions until a routine level of performance is achieved. This approach is very much dependent on expert guidance and assessment. Achieving excellent performance requires expert mentoring[11] but in technical-medicine, experts to learn from are scarce, therefore, a different didactic approach is needed which makes learners responsible for their own learning process and assessment using principles based on interdisciplinary learning and expertise.[47] The principles of self-assessment, self-directed learning and reflective practice are underlying this didactic approach.
Outlook and future directions
The technological transformation of healthcare calls for specifically trained technical-medical experts to reduce the misuse of medical technology and improve the quality of care for patients. Hybrid curricula, such as the Technical Medicine program, can bridge the gap between medicine and technology. We argued that adaptive and interdisciplinary expertise should be underlying concepts of developing technical-medical expertise. In the future, structured and systematic investigations should be performed on how this technical-medical expertise develops over time, how technical physicians learn to integrate technical and medical competencies and what a curriculum should look like to optimally support the development of adaptive and interdisciplinary expertise. Insights from these investigations can be used by curriculum designers and other stakeholders for curriculum development, both in initial (higher) education, but also in continuing professional development.
Several studies have demonstrated the clinical impact of technical physicians by looking at the practice of technical physicians[48][49] and the medical specialists’ perceptions of the impact on clinical practice.[8] Further investigations of technical physicians’ performance are needed, and we agree with De Haan et al.[48] that this should be done without directly comparing it to an established group because they do different things. One of the major remaining questions is how patients perceive the care provided by technical physicians.
Acceptance of technical physicians in clinical practice is not self-evident. The acceptance and embedding of this new profession still depend too much on the willingness of individual physicians, other healthcare professionals and healthcare insurers.[48] Removing the organizational and social barriers in clinical practice as identified by De Haan et al.[49] and Groenier et al.[8] should therefore be a priority for policymakers.
Clinical practice is inherently interdisciplinary and interdisciplinary collaboration, especially when it involves medical technology, can contribute to better healthcare.[36][50] However, interdisciplinary teamwork is not easy to accomplish. The introduction of new professions in healthcare, such as technical physicians, requires rethinking who is qualified and competent for certain procedures,[8] vertically and horizontally shifting tasks[48] and shifting roles and responsibilities. This changing healthcare system affects the training of all healthcare professionals and how they work together. The introduction of the technical physician therefore necessitates a rethinking of roles and a focus on interdisciplinary collaboration for the training of all healthcare professionals.
References
- Fuchs VR, Sox Jr HC. Physicians’ views of the relative importance of thirty medical innovations. Health Aff. 2001;20(5):30-42.[↑]
- Aarts S, Cornelis F, Zevenboom Y, et al. The opinions of radiographers, nuclear medicine technologists and radiation therapists regarding technology in health care: a qualitative study. J Med Radiat Sci. 2017;64(1):3-9.[↑][↑]
- Rambukwella M, Balamurugan A, Klapholz H, Beninger P. The application of engineering principles and practices to medical education: Preparing the next generation of physicians. Med Sci Educ. 2021;31:897-904. doi:10.1007/s40670-021-01217-x/Published[↑][↑][↑][↑][↑]
- Green CA, Mahuron KM, Harris HW, O’Sullivan PS. Integrating robotic technology into resident training: Challenges and recommendations from the front lines. Academic Medicine94. 2019;94(10):1532-1538. doi:10.1097/ACM.0000000000002751[↑]
- Hague CM, Merrill SB. Integration of robotics in urology residency programs: An unchecked technological revolution. Curr Urol Rep. 2021;22:47. doi:10.1007/s11934-021-01062-w[↑]
- Overton KD, Coiado O, Hsiao-Wecksler ET. Exploring the intersection of engineering and medicine through a neuroscience challenge laboratory. Med Sci Educ. 2022;32:1481-1486. doi:10.1007/s40670-022-01676-w[↑][↑]
- World Health Organization. Medical Devices: Managing the Mismatch: An Outcome of the Priority Medical Devices Project. World Health Organization; 2010.[↑]
- Groenier M, Spijkerboer K, Venix L, et al. Evaluation of the impact of technical physicians on improving individual patient care with technology. BMC Med Educ. 2023;23(1):1-9. doi:10.1186/S12909-023-04137-Z/TABLES/3[↑][↑][↑][↑]
- Groenier M, Pieters JM, Miedema HAT. Technical Medicine: Designing medical technological solutions for improved health care. Med Sci Educ. 2017;27:621-631. doi:10.1007/s40670-017-0443-z[↑][↑][↑][↑][↑][↑][↑]
- Ericsson KA, Lehmann AC. Expert and exceptional performance: Evidence of maximal adaptation to task constraints. Annu Rev Psychol. 1996;47(1):273-305. doi:10.1146/annurev.psych.47.1.273[↑][↑][↑][↑]
- Ericsson KA. Deliberate practice and acquisition of expert performance: A general overview. Academic Emergency Medicine. 2008;15:988-994. doi:10.1111/j.1553-2712.2008.00227.x[↑][↑][↑][↑]
- Chi MTH. Two approaches to the study of experts’ characteristics. In: Ericsson KA, Charness N, Feltovich P, Hoffman R, eds. The Cambridge Handbook of Expertise and Expert Performance. Cambridge University Press; 2006:21-30. doi:10.1017/CBO9780511816796.002[↑][↑][↑]
- Chi MTH, Glaser R, Farr MJ. The Nature of Expertise. Erlbaum Associates; 1988.[↑][↑][↑]
- Schraagen J. The Generality and Specificity of Expertise. PhD thesis. University of Amsterdam; 1994.[↑]
- Ericsson KA. The influence of experience and deliberate practice on the development of superior expert performance. In: Ericsson KA, Charness N, Feltovich P, Hoffman R, eds. The Cambridge Handbook of Expertise and Expert Performance. Cambridge University Press; 2006:685-705. doi:10.1017/CBO9780511816796.038[↑]
- Fadde PJ, Klein GA. Deliberate performance: Accelerating expertise in natural settings. Performance Improvement. 2010;49(9):5-14. doi:10.1002/pfi.20175[↑][↑][↑][↑][↑][↑]
- Graber ML, Franklin N, Gordon R. Diagnostic error in internal medicine. Arch Intern Med. 2005;165(13):1493-1499. doi:10.1001/archinte.165.13.1493[↑]
- Van Tartwijk J, Zwart R, Wubbels T. Developing teachers’ competences with the focus on adaptive expertise in teaching. In: Clandinin D, Husu J, eds. The SAGE Handbook of Research on Teacher Education. Vol 2. Sage; 2017:820-835.[↑]
- Lehtinen E, Gegenfurtner A, Helle L, Säljö R. Conceptual change in the development of visual expertise. Int J Educ Res. 2020;100:101545. doi:10.1016/J.IJER.2020.101545[↑]
- Charlin B, Tardif J, Boshuizen HP. Scripts and medical diagnostic knowledge: theory and applications for clinical reasoning instruction and research. Acad Med. 2000;75(2):182-190. doi:10.1097/00001888-200002000-00020[↑]
- Dijkstra S, Merriënboer J. Plans, procedures, and theories to solve instructional design problems. In: Dijkstra S, Seel N, Schott F, Tennyson R, eds. Instructional Design International Perspective: Solving Instructional Design Problems . Vol 2. Lawrence Erlbaum Associates; 1997:23-44.[↑][↑][↑]
- Schmidt HG, Boshuizen HPA. On acquiring expertise in medicine. Educ Psychol Rev. 1993;5(3):205-221.[↑]
- Elstein AS, Schwartz A. Clinical problem solving and diagnostic decision making: selective review of the cognitive literature. Br Med J. 2002;324(March):729-732. doi:10.1136/bmj.324.7339.729[↑]
- Mylopoulos M, Regehr G. Cognitive metaphors of expertise and knowledge: Prospects and limitations for medical education. Med Educ. 2007;41(12):1159-1165. doi:10.1111/j.1365-2923.2007.02912.x[↑][↑][↑]
- Ericsson KA. Deliberate practice and the acquisition and maintenance of expert performance in medicine and related domains. Acad Med. 2004;79(10 Suppl):S70-S81. doi:10.1097/00001888-200410001-00022[↑]
- Wits W, Homminga J, Endedijk M, et al. Teaching design engineering in an interdisciplinary programme. In: Proceedings of the 16th International Conference on Engineering and Product Design Education. University of Twente; 2014.[↑][↑][↑]
- Koen B. Definition of the Engineering Method. ASEE Publications; 1985.[↑]
- Goel V, Pirolli P. The structure of design problem spaces. Cogn Sci. 1992;16(3):395-429. doi:10.1016/0364-0213(92)90038-V[↑]
- Darrow JJ, Avorn J, Kesselheim AS. FDA approval and regulation of pharmaceuticals, 1983-2018. JAMA. 2020;323(2):164-176. doi:10.1001/jama.2019.20288[↑]
- Wagner MV, Schanze T. Challenges of medical device regulation for small and medium sized enterprises. Current Directions in Biomedical Engineering. 2018;4(1):653-656. doi:10.1515/CDBME-2018-0157/MACHINEREADABLECITATION/RIS[↑]
- Palonen T, Boshuizen HPA, Lehtinen E. How expertise is created in emerging professional fields. Promoting, assessing, recognizing and certifying lifelong learning: International perspectives and practices. Published online 2014:131-150. doi:10.1007/978-94-017-8694-2_8[↑]
- Hatano G, Inagaki K. Two courses of expertise. In: Stevenson HW, Azuma H, eds. Child Development and Education in Japan. W. H. Freeman & Co.; 1986:262-272.[↑]
- Schwartz D, Bransford JD. Efficiency and Innovation in Transfer. Transfer of Learning from a Modern Multidisciplinary Perspective. 2005;(3):1-51. doi:10.1111/j.1365-2133.2005.06492.x[↑]
- Bohle Carbonell K, Stalmeijer RE, Könings KD, Segers M, van Merriënboer JJG. How experts deal with novel situations: A review of adaptive expertise. Educ Res Rev. 2014;12:14-29. doi:10.1016/j.edurev.2014.03.001[↑][↑]
- Kua J, Lim WS, Teo W, Edwards RA. A scoping review of adaptive expertise in education. Med Teach. 2021;43(3):347-355. doi:10.1080/0142159X.2020.1851020/SUPPL_FILE/IMTE_A_1851020_SM4935.DOCX[↑]
- Boon M, van Baalen S, Groenier M. Interdisciplinary expertise in medical practice: Challenges of using and producing knowledge in complex problem-solving. Med Teach. 2019;41(6). doi:10.1080/0142159X.2018.1544417[↑][↑][↑][↑][↑][↑]
- Lisk K, Agur AMR, Woods NN. Examining the effect of self-explanation on cognitive integration of basic and clinical sciences in novices. Advances in Health Sciences Education. Published online 2016:1-13. doi:10.1007/s10459-016-9743-0[↑]
- Kulasegaram KM, Grierson LEM, Norman GR. The roles of deliberate practice and innate ability in developing expertise: evidence and implications. Med Educ. 2013;47(10):979-989. doi:10.1111/medu.12260[↑][↑]
- Miedema HAT. Arts En Ingenieur, and Ever the Twain Shall Meet: Analyse En Ontwerp van de Opleiding Technische Geneeskunde. University of Twente; 2015. doi:10.3990/1.9789036539487[↑]
- Ormel B, Pareja Roblin N, McKenney S, Voogt J, Pieters J. Research–practice interactions as reported in recent design studies: still promising, still hazy. Educational Technology Research and Development. 2012;60:967-986.[↑]
- Goldberg D, Somerville M. A Whole New Engineer: The Coming Revolution in Engineering Education. Threejoy; 2014.[↑]
- Shön D. The Reflective Practitioner. Temple Smith; 1983.[↑][↑]
- Groenier M. The Decisive Moment: Making Diagnostics Decisions and Designing Treatments. PhD thesis. University of Twente; 2010.[↑]
- Ericsson KA, Krampe RT, Tesch-Römer C. The role of deliberate practice in the acquisition of expert performance. Psychol Rev. 1993;100(3):363-406. doi:10.1037/0033-295X.100.3.363[↑]
- Ward P, Gore J, Hutton R, Conway GE, Hoffman RR. Adaptive skill as the conditio sine qua non of expertise. J Appl Res Mem Cogn. 2018;7(1):35-50. doi:10.1016/J.JARMAC.2018.01.009[↑]
- Halfwerk F, Groot Jebbink E, Groenier M. Development and evaluation of a proficiency-based and simulation-based surgical skills training for Technical Medicine students. MedEdPublish. 2020;9(1). doi:10.15694/MEP.2020.000284.1[↑]
- Miedema H, Groenier M. Training adaptive endoscopic surgeons: the didactical paradox. In: Broeder I, Kalisingh S, Perretta S, Szold A, eds. The Technical Principles of Endoscopic Surgery. Bohn Stafleu Van Loghum; 2024:1-10.[↑]
- De Haan Id M, Van Eijk-Hustings Y, Bessems-Beks M, De Bruijn-Geraets D, Dirksen C, Vrijhoef H. Evaluating task shifting to the clinical technologist in Dutch healthcare: A mixed methods study. PLoS One. 2023;18(3):e0281053. doi:10.1371/journal.pone.0281053[↑][↑][↑][↑]
- de Haan M, van Eijk-Hustings Y, Bessems-Beks M, Dirksen C, Vrijhoef HJM. Facilitators and barriers to implementing task shifting: Expanding the scope of practice of clinical technologists in the Netherlands. Health Policy (New York). 2019;123(11):1076-1082. doi:10.1016/j.healthpol.2019.07.003[↑][↑]
- Becker EA, Schell KS. Understanding, facilitating, and researching interprofessional education. Respir Care. 2017;62(7):999. doi:10.4187/respcare.05678[↑]
